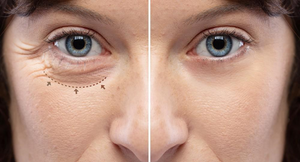
Understanding Xanthelasma: the weird yellow deposits on your eyelids!
Do you suddenly notice strange yellow bumps on your eyelids? You may have what is called Xanthelasma.
Read this blog to understand the condition, causes, and treatment options.
Let’s dive right in!
What is Xanthelasma?
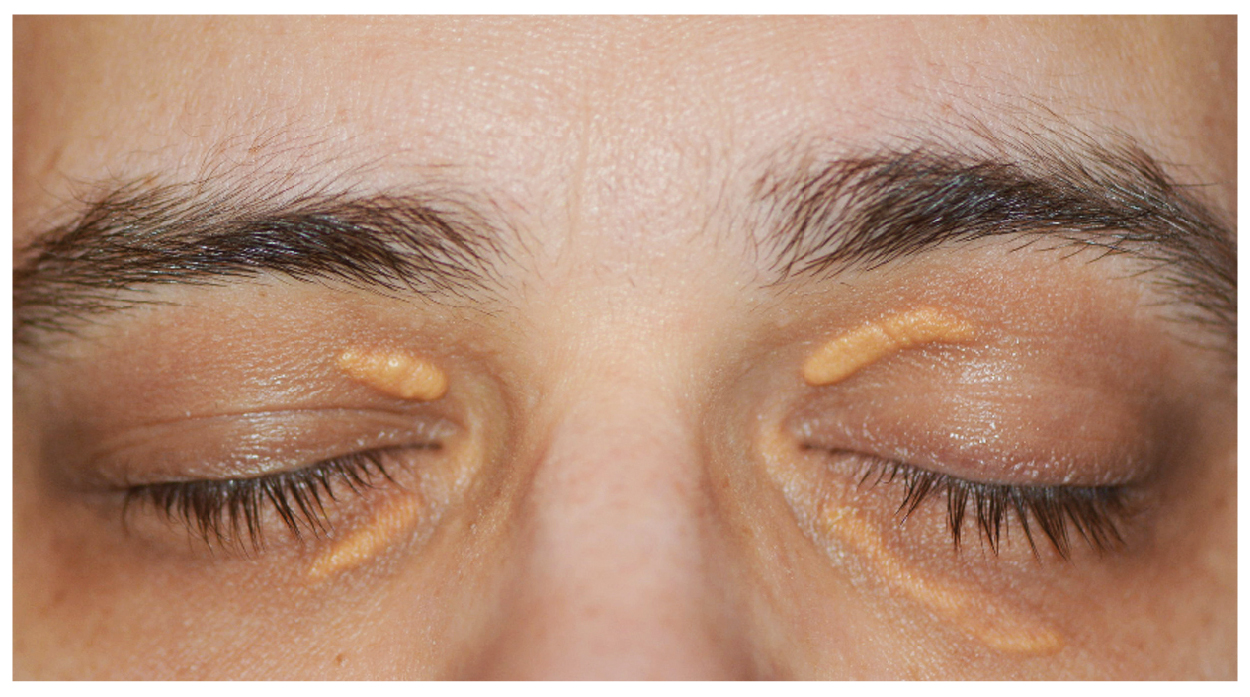
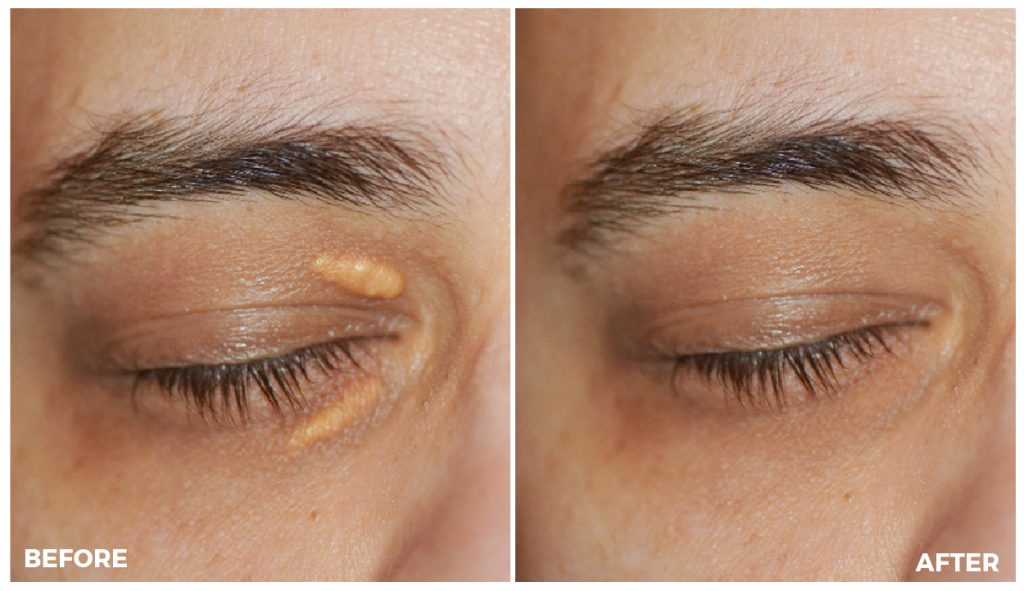
Xanthelasma is a common skin condition characterised by yellow, raised plaques on the eyelids. The plaques are made up of cholesterol deposits and can vary in size, shape, and number. Xanthelasma is not harmful but can cause cosmetic concerns.
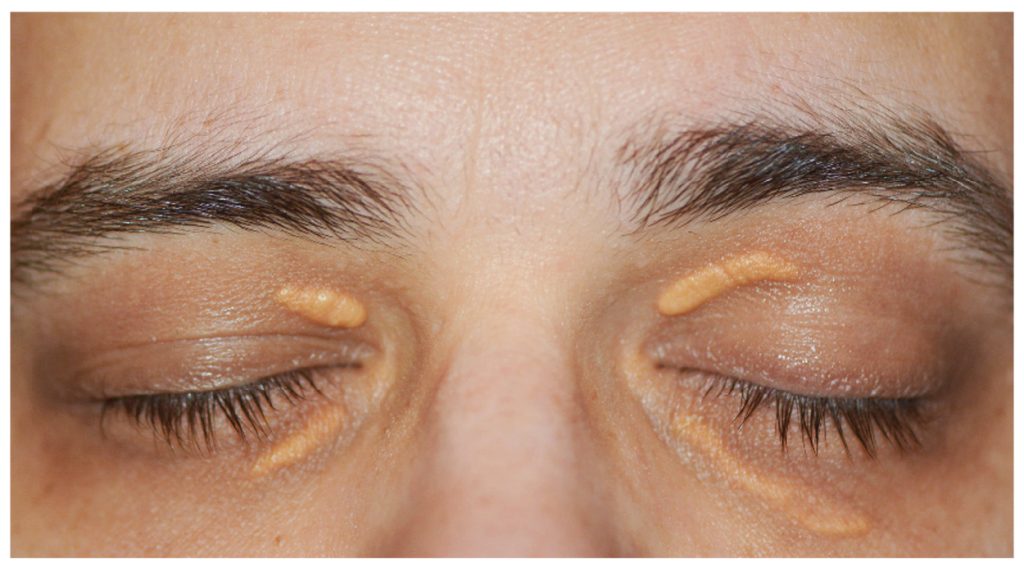

Xanthelasma is most found in middle-aged and older individuals and is more common in women. It is also more prevalent in people of Asian, Mediterranean, and Middle Eastern descent. People with high cholesterol, high triglycerides, or other lipid disorders are more likely to develop Xanthelasma. Additionally, those with a genetic predisposition to high cholesterol may be more likely to develop Xanthelasma.
It is important to note that sometimes Xanthelasma can also be seen in individuals with normal lipid levels, and it’s not always clear what causes it.
What are the common symptoms associated with Xanthelasma?
The main symptom of Xanthelasma is the presence of yellow, raised plaques on the eyelids, typically on the inner corner of the eye near the nose. These plaques may be symmetrical and may appear on one or both eyelids. They can vary in size and shape but are usually small (less than 1 cm in diameter) and have a well-defined border.
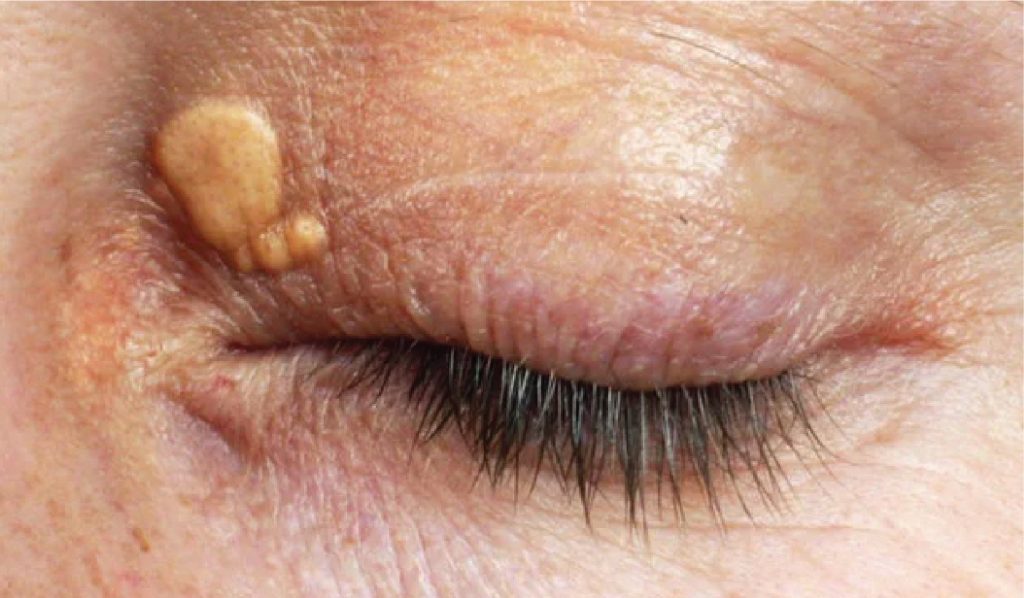

Other common symptoms of Xanthelasma include:
- A change in the colour of the skin around the plaques
- A change in the texture of the skin around the plaques
- Itching or burning sensation around the plaques
- Soreness or tenderness around the plaques
Xanthelasma can significantly impact self-esteem because it is a visible skin condition typically located on the face, specifically on the eyelids. The yellow, raised plaques can be noticeable and cause embarrassment and self-consciousness.
Some people may feel self-conscious about their appearance and avoid social situations or activities where their Xanthelasma is likely to be seen. They may think their Xanthelasma makes them look unhealthy or unattractive, which can negatively impact self-esteem.
Additionally, Xanthelasma can also cause emotional distress, such as anxiety, depression, and feelings of low self-worth. For some people, it can even affect their professional lives.
It is important to note that everyone’s experience with Xanthelasma is unique, and the impact on self-esteem can vary widely. Some people may not be affected by the condition, while others may feel significantly impacted. Consulting an oculoplasty surgeon or a mental health professional can help in managing the emotional and psychological impact of Xanthelasma.
What are Xanthelasma treatment options?
Treatment options for Xanthelasma removal include:
- Cryotherapy: This involves freezing the Xanthelasma with liquid nitrogen. Cryotherapy is a relatively simple and inexpensive method, but it can cause scarring and discolouration of the skin.
- Surgical excision involves cutting out the Xanthelasma with a scalpel or laser. Surgical excision is a more invasive method than cryotherapy. Still, it is more effective in removing the Xanthelasma and is less likely to cause scarring.
- Topical creams: Topical creams containing retinoids or alpha-hydroxy acids can soften and reduce the size of the Xanthelasma. These creams are relatively non-invasive but may take a long time to be effective.
- Chemical Peels: Chemical peels containing glycolic acid, salicylic acid, or trichloroacetic acid can be used to exfoliate the skin, reducing the size of Xanthelasma.
- Laser treatment for Xanthelasma: is reasonably effective without causing much damage to the surrounding skin. But it may require multiple sessions, and the Xanthelasma removal cost is relatively high.
Are these treatments successful?
The Xanthelasma treatments mentioned above have risks and limitations, including
- the need for multiple sessions
- cost
- secondary pigmentation, lid deformities, and scarring due to insufficient depth penetration or too deep
- 30% risk of recurrence. All Xanthelasma cells need to be removed to avoid recurrence, which may not be possible with the abovementioned treatments
Is there an innovative way to treat Xanthelasma?
Plexr Pro is the latest innovation that uses plasma to sublimate tissues. This machine is manufactured by GMV (Italy). Plasma, a term derived from the Greek language for ”entity” or ”form”, is the fourth state of matter. It consists of negatively charged electrons and positively charged ions with a net neutral charge.
Plexr Pro generates plasma like a bolt of micro lightning that acts only on the skin’s outer layer. Before sublimating, the skin cells transmit a selective estimated quantity of energy in the form of heat, to the dermis’ proper deepness, without irradiation (laser/light) or electric shock (electrosurgical unit /current). No form of energy is delivered directly from the device to the deeper tissue; no eddy currents are generated.
It is a non-invasive, non-ablative, outpatient department technique, where the air between the tip of Plexr Pro and the skin produces plasma from atmospheric gas. This focused microbeam sublimates the targeted tissue without damaging the surrounding areas. The tissue destruction is precise and controlled.
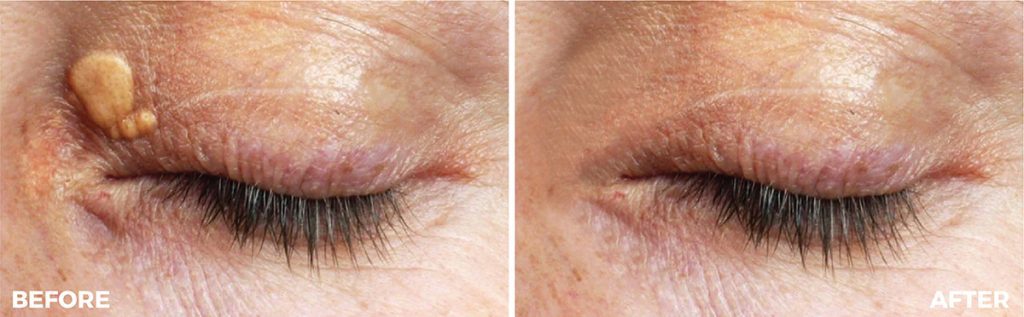

What are the advantages of this technique?
Plexr Pro is a portable device, easy to use and ideal for office use. The advantages of this technique include excellent efficacy, minimal downtime, increased safety, and predictability of results. The cost of the treatment is affordable, and the risk of damage to the eye is minimal. The other advantages of this energy are immediate contraction of the collagen fibres, collagen reorganisation, formation of new collagen, and renewal of the epidermal tissue. Hence, there is no scar or residual contraction at the site of lesion removal.
How is it done?
It is an outpatient procedure done under topical anaesthesia. Usually, 1 to 3 sittings are required, especially for larger XPs where multiple layers may need to be removed. The procedure time is at most 15 to 20 min for both eyes. The spray technique is used to sublimate the XP deposit layers and clean carbonised skin particles.
What kind of post-procedure care is required?
The procedure may cause minor oedema and redness, persisting for a week or so. Patients are advised not to use water near the site for 24 hours, to clean the face with medicated cleansers, and use Vitamin K and sunscreen loaded with Zinc oxide. It is also recommended to avoid exposure to the sun.
What can a patient expect from the procedure?
There may be scab formation in the localised areas of the XP deposit, which usually falls off and the new epidermis scaffolds over without any scar formation.
Are there any recurrences with Plexr Pro?
Plexr Pro is a reasonably new treatment modality for XPs. However, a study by Rubins et al. in 2019, amongst 15 patients with XP, indicates a 100% clearance of lesions with just a single treatment. All the wounds were re-epithelialized within 1 to 2 weeks of treatment. There were no reports or evidence of scarring, dyspigmentation, or recurrence up to 12 months post-procedure. The patients expressed complete satisfaction with the cosmetic outcomes of their treatments, with no reports of pain or discomfort during or after the procedure.
In conclusion, Xanthelasma is a complex condition. While various treatment options are available, Plasma Plexr Pro is a cheaper, more reliable, non-invasive, and more predictable alternative to consider.

How to prevent Xanthelasma?
There is no sure-fire way to prevent Xanthelasma. Still, there are some steps you can take to reduce your risk of developing the condition. These include
- so taking steps to manage your cholesterol levels, such as eating a healthy diet, getting regular exercise, and taking cholesterol-lowering medications as prescribed, may help to prevent the condition.
- Controlling blood sugar levels: Diabetes is another risk factor for Xanthelasma, so controlling your blood sugar levels through diet, exercise, and medication can help to reduce your risk.
- Protecting your skin from UV rays: Sun exposure can cause damage to the skin, which may increase your risk of developing Xanthelasma. Wearing sunscreen and protective clothing when spending time outdoors can help to protect your skin from UV rays.
- Not smoking: Smoking can increase your risk of Xanthelasma, so quitting smoking can help reduce your risk.
- Manage other medical conditions: Other medical conditions like hypertension, obesity, and liver disease may also increase your risk of developing Xanthelasma. Managing these conditions through treatment and lifestyle changes may help to prevent the condition.
It’s important to note that Xanthelasma can also develop with no known risk factors, so there is no guarantee following these steps will prevent it. However, these steps may help to reduce your risk of developing Xanthelasma or other health problems.
Can I get Xanthelasma treatment near me?
Yes, Clinica Fai, India’s leading 360-degree eye and face plastic surgery clinic, with its flagship store in Jubilee Hills, Hyderabad, is the first clinic in India to offer Plasma Plexr-based Xanthelasma treatment. Dr Shubhra Goel, the CEO and Chief Surgeon at Clinica Fai, is one of India’s top celebrity oculofacial plastic surgeons. She is the key opinion leader for Plasma Plexr and has been offering the best treatment for Xanthelasma in India.